Medtech regulation outlook in 2023: Faster approvals among priorities as AI moves to fore
For medical device makers – and the patients who rely on them – 2023 is poised to be a year of challenge and change for regulation.
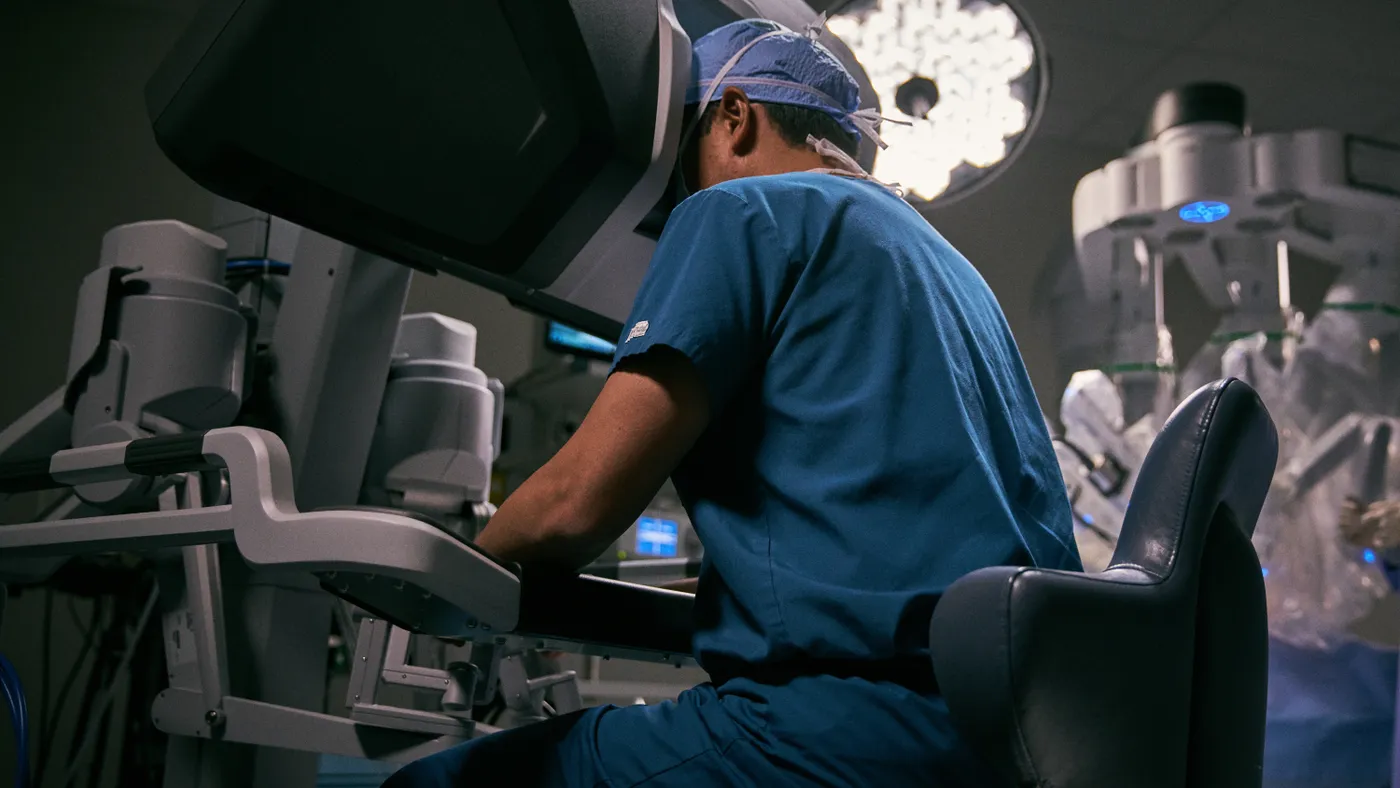
A post-COVID-19 surge in applications for review and the burgeoning role of artificial intelligence and machine learning — combined with swift advances in monitoring technology and wearable sensors — have pushed digital health to the fore.
That’s forcing the Food and Drug Administration to conceive of new ways to address the safety of devices that are continuously updating or even learning on the job.
In Europe, the European Commission has delayed its implementation of Medical Device Regulation and In-Vitro Device Regulation, while numerous industry observers there fear there won’t be enough capacity to review new and existing devices before the latest deadline arrives.
MedTech Dive asked industry observers in the medtech field for their view on the regulatory challenges facing the sector and the regulators themselves in 2023:
Andrew Fish, president and CEO of the Medical Device Innovation Consortium: The FDA has some key challenges that include both overall workload and developing new regulatory approaches to better address evolving and emerging technologies. On workload, the COVID pandemic brought its own challenges with a huge number of submissions for emergency use authorizations and related work for the agency. The agency is now emerging from that crush, but will have to continue dealing with the challenge of hiring, training and retaining enough staff to stay on top of applications. The recent five-year reauthorization of the Medical Device User Fee Amendments is designed to both set review timeline goals for the agency and provide sufficient funding to support the agency’s medical device review function.
Much of our work at the Medical Device Innovation Consortium, which we do in close in collaboration with FDA as a member of our public-private partnership, is focused on advancing medical device regulatory science to help improve the quality of device submissions and expedite the review process by leveraging modernized approaches to evidence development. Advances like these make it easier for reviewers to efficiently and confidently assess safety and efficacy.
Another fundamental challenge is the pressure that evolving and novel technologies put on the regulatory system in terms of how to evaluate device safety and efficacy in the context of new functions and the proliferation of devices that generate and leverage data. The FDA has wrestled, for example, with how to regulate machine learning software in medical devices because its regulatory review approach is rooted in a one-time approval of a static, unchanging device that often requires a new review of any device modifications. That’s not an approach that moves quickly and doesn’t easily accommodate the great potential benefit of machine learning in medical devices in making fast-paced iterative improvements. So that’s an example of how the agency is challenged to regulate at the speed of innovation and unleash the full potential of the medtech revolution, while still providing assurances of safety and efficacy and finding the optimum outcome for patients and public health. These are the kinds of challenges that MDIC was created to address, by bringing together regulators, manufacturers, and a wide range of stakeholders to develop collaborative solutions that accelerate patient access to medical technologies that save lives and improve quality of life.
Rachel Sher, attorney specializing in FDA regulation with the legal and consulting firm Manatt in Washington, DC: Congress has spoken: FDA and medical product sponsors must make more progress toward the goal of ensuring better participation in clinical trials by diverse and underserved populations. The Food and Drug Omnibus Reform Act of 2022 (FDORA) established a new requirement that all marketing applications for medical devices and drugs include a “diversity action plan” detailing the ways in which sponsors will meet specified enrollment goals.
The COVID-19 pandemic underscored the promise that decentralized clinical trials hold in helping to foster greater clinical trial participation by all patients. The continued success of the decentralized clinical trial model relies on more and better use of digital health technologies, like smart and wearable devices. As these technologies evolve, FDA must continue to iterate on the guidance it has issued to date to ensure that developers in this space can speed products that meet FDA’s standards to patients and all of those engaged in the clinical trial enterprise.
Larissa D’Andrea, vice president, Government Affairs, Market Access and Clinical Affairs, ResMed: 2023 is a critical year for digital health in the European Union and the United States, particularly around how policy will affect how digital health is prescribed, administered and, ultimately, further adopted.
In the United States, the pandemic fundamentally accelerated the utilization of telemedicine. For the benefit of the patient, we should build on that momentum through the creation of permanent digital/virtual care pathways that improve patient access and health.
In the EU, I strongly support the opportunity to create consistency around data capture and use, plus privacy regulations that both protect patients and enable their use of digital health solutions.
I am looking forward to working with our legislative, regulatory, payor and distribution partners to advance this agenda on behalf of patients globally.
David Kunz, senior vice president, Global Quality, Clinical and Regulatory Affairs at Zimmer Biomet: Our initial focus items for 2023 with regard to the U.S./EU regulatory horizon are looking for continued progress on EU Medical Device Regulations (MDR) and dealing with resource constraints at notified bodies [the national testing firms or laboratories that certify medical devices in the EU]. We’re also looking closely at supply chain challenges that are driving the need for rapid product change approvals to avoid product supply shortages. Standard regulatory review timelines will limit responsiveness to supply chain challenges.
Roz Burke, senior vice president, Global Quality and Regulatory at Boston Scientific: When we talk about patient safety in a regulatory context, we’re really talking about two things: ensuring that available devices and therapies are safe and effective, and ensuring that industry can continue to develop new solutions for unmet clinical needs to save lives and improve quality of life. It’s vital that the relationship between industry and regulators prioritizes both of these so that we can continue to enable meaningful changes in patients’ lives.
In the U.S., the FDA’s willingness to look at new technologies and rethink traditional submission periods has helped industry to move much more quickly toward superior quality technologies. Machine-based and automated inspection have the potential to offer more robust safeguards than human inspection for certain tasks, and FDA has been thoughtful in how they validate and expedite traditional review periods in light of new technologies becoming available. We look forward to the continued evolution of these approval pathways to encourage broader adoption of these technologies.
We’re also optimistic about the agency’s commitment to agility, especially with regard to software validation and digital health applications. The use of real-time, real-world data and advanced algorithms is turning traditional paradigms on their heads, and we need a more agile approach to maintain strong, effective oversight while responding to patient and physician needs in an increasingly dynamic marketplace.
In Europe, we welcomed the recent publication of the European Commission’s proposal to amend transitional measures in the EUMDR. While we were well-positioned to comply, we recognize the likelihood of challenges for the medical device innovation ecosystem, including costly implementation challenges that could prove prohibitive for many smaller players and logistical hurdles with fewer Notified Bodies to process an influx of submissions.”
Agata Anthony, vice president, head of Global Regulatory Affairs, GE HealthCare:
In Europe, the most important regulatory development in the medical device space is the anticipated change in the implementation of Medical Device Regulation (MDR). Due to concerns with the ability of Notified Bodies to process the vastly increased demand for audits and certifications and potential for significant disruption to availability of medical technologies in the European market, the legislators are considering a proposal to modify the implementation date for the MDR from 2024 to 2027-2028, depending on device class. This is an encouraging development and if adopted will enable a smoother transition to the new requirements.
In the U.S., the recently passed Omnibus funding bill expanded FDA’s authority in enforcing requirements to assure cybersecurity of medical devices. This will enable the Agency to verify that new technologies submitted after the law comes into force contain cybersecurity protections, and that manufacturers have a plan to manage those devices and provide patches throughout the product life cycle.
Another significant trend relates to the rapid growth in devices utilizing Artificial Intelligence and Machine Learning. The FDA signaled that a guidance document describing use of algorithm change protocols is on the list of guidance priorities for 2023. This guidance would describe the types of changes, which could under certain conditions be implemented without the need to file an additional submission. This would be an important development for innovative AI/ML technologies, as it allows the faster pace of innovation to proceed while maintaining appropriate regulatory oversight.
Updates with comments from Andrew Fish, president and CEO of the Medical Device Innovation Consortium