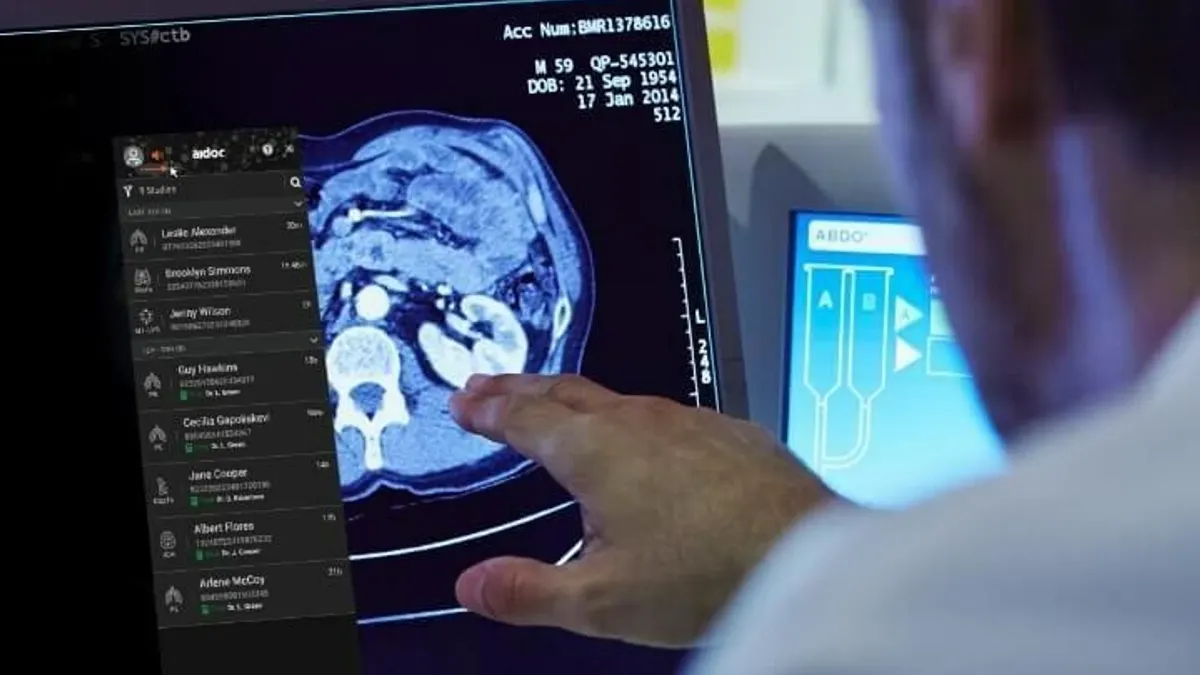
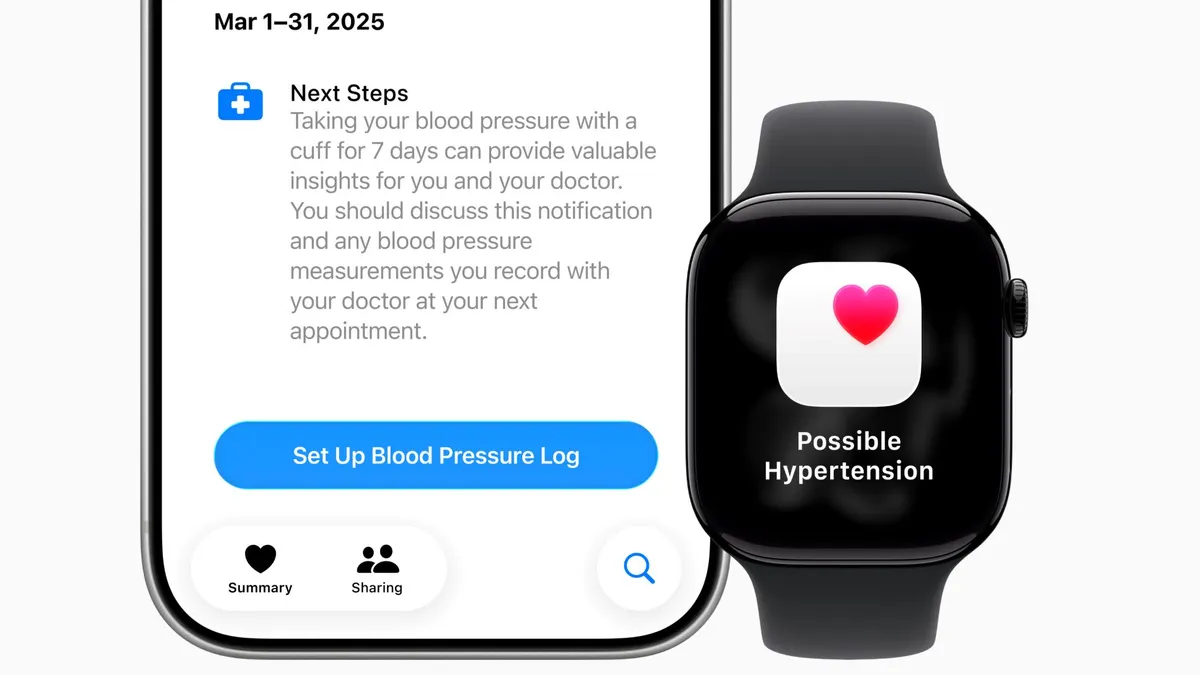
Medical urgency, advances in technology and reimbursement changes during the pandemic have expanded the use of remote patient monitoring. More patients with implantable and wearable devices are connecting with their doctors via smartphone apps, enabling earlier detection of changes in health conditions.
Medtronic last year decided the time was right to sell or spin off its patient monitoring business, along with its respiratory care operations. Now in the midst of that process, the company has been mum on next steps in divesting the businesses, which together generate $2.2 billion in annual revenue.
Medtronic CEO Geoff Martha, in announcing the separation plan in October, said it would help Medtronic focus on opportunities better aligned with its long-term strategies for accelerating growth and would position the new company to unlock value.
“Independently, NewCo will be a leading connected care company with a compelling leadership position, attractive margins, and potential for growth acceleration with increased investment and dedicated capital allocation," Martha said at the time.
Dr. Sam Ajizian, Medtronic’s chief medical officer for patient monitoring, talked to MedTech Dive about the business’s growing partnership with BioIntelliSense, whose wearable BioButton provides continuous remote monitoring of vital signs, and about the opportunities to transform patient treatment through connected care.
This interview has been edited for length and clarity.
MEDTECH DIVE: What factors, across the healthcare landscape, are accelerating the shift to connected care?
AJIZIAN: We have to have an infrastructure that can meet many needs in the medical community. Post COVID, we've lost a great deal of nursing providers and physician providers, as well as other allied health professionals, pharmacists and respiratory therapists. We know that the patients haven't gone away. In fact, we know that acuity – how sick patients are – is increasing on that general care floor.
When you have sicker patients and less caregivers, there's a gap there. And right now, we basically assess vital signs on the general ward the same way we did about 100 years ago, manually going in and taking a set of vital signs. We used to write it on a piece of paper that stayed at the foot of the bed. Now it goes into a big expensive electronic medical record, but the process is still largely manual, and we only get about four to six data points a day as providers on which to base decisions.
Now, we have the opportunity, through really good technology, to not only keep patients safe with continuous monitoring on the ward, but also improve workflow around manual collection of vital signs, freeing up providers on the ward to do the nursing care that they went into the profession for, right? Be at the bedside, and put hands on and help patients get better, rather than common administrative tasks that we can automate.
If this technology isn't connected [through] electronic medical records to providers in whatever mode they want, it's not going to be scalable. So we're really focusing on solutions that connect easily in the medical technology biosphere, and that includes the electronic medical record and other devices in the hospital as well as data to help drive an AI, machine-learning engine so that we as providers can act earlier based on early trending, rather than just lines in the sand, reacting to an alarm that goes off.
How are you incorporating AI into connected care?
AI in healthcare is one of the biggest growth areas that we're seeing globally right now. It's coming in a lot of forms. For us in the patient monitoring business, we're really focusing on using our existing technologies and new technologies to harvest the physiologic data that these devices are giving out continually. And then as I said earlier, converting them into ways for providers to act earlier.
The real value of AI in patient monitoring is taking a reactive device that alarms for a threshold and converting it into a predictive and preventive physiologic trend. What that means is that, if a patient's got a fever and a rash and a cough, I can look at them and figure out what's wrong. What we're trying to do is, before symptoms that are that obvious arise, use physiologic data trends to warn providers that concerning trends are developing.
With continuous trending and machine learning and AI algorithms based on lots of data, we can develop an actionable way to intervene earlier, and earlier is better for any disease process. Earlier is simply better outcomes.

Sam Ajizian
Chief medical officer for patient monitoring at Medtronic
There's already plenty of data around this. Coming out of the pandemic, people were able to look at vital sign changes with wearable technology before patients developed COVID. These are what we call early pathophysiologic signatures, meaning providers cannot see them with the standard methods that we use: a set of vitals, an exam, maybe some lab work. But we know that with continuous trending and machine learning and AI algorithms based on lots of data, we can develop an actionable way to intervene earlier, and earlier is better for any disease process. Earlier is simply better outcomes, less expensive, and easier to do in a lower acuity setting, like a general care floor or even at home.
How much AI-based intervention is happening now, and how much is still a ways off?
There is a lot of work to be done here, in scaling this to many different disease states, patient cohorts and the like. That is the downstream part of work that will be done and deployed in the next few years. But right now we have the ability to do continuous monitoring on the general care floor and even at home and pick up basic trends that are maybe not disease-specific, but are certainly able to warn you that a concerning trend is developing. That allows the care team to intervene earlier.
For example, a patient could be on the general care floor, getting their vital signs monitored continuously instead of every six hours. A trend is developing in, let's say, increasing respiratory rate, and maybe increase in temperature or heart rate in that six-hour interval that the continuous monitoring sees. The AI in the algorithms notices that trend, notifies providers, and then it's up to us as providers to say, oh goodness, I'm a little worried about this patient. Perhaps they're developing an infection, or perhaps they're developing some atelectasis in their lungs. And while I may not be able to see a significant disease process yet, I know something is developing. So I can do some early interventions like starting oxygen, perhaps getting them out of bed and ambulating them, perhaps drawing some blood, or simply going back a little more frequently to look at them, versus six hours go by or longer and a trigger occurs that is far more down the stream of the disease process development.
And that's what we want to avoid. As much as we're really good as intensive care doctors, like myself, running upstairs to the ward and saving someone and bringing them to the ICU, we want to get out of that business. We want to get into the business of taking care of those patients before they require the critical care. So that work is out there now, it is starting. And it's going to mature as time goes on to the final state of what we would call personalized medicine, where the system knows you, what your baseline vitals are, what your trends are. That can help inform the physician when you do come into the hospital, what your baseline is and how you deviated from it. So we'll open up a new way of caring for people earlier in the disease process that's, quite frankly, very exciting.
What are the capabilities of the wearable from Medtronic’s partner BioIntelliSense?
We're distributing the BioIntelliSense BioButton now, which is a small device worn under the collarbone with a sticker that monitors those parameters, and it can monitor indefinitely because it's a rechargeable device. The device connects either in the hospital or at home through a very simple gateway. It has incredibly simple human factors. So we're confident it can be deployed easily in the home with the most minimal instructions, and we are very excited about partnering with healthcare systems wanting to bring care into the home, keep patients out of the hospital, get them out sooner, but also keep them safe while they're inside the hospital. That BioButton can be applied when you're in the hospital on the [medical/surgical] ward, taking you from intermittent vital signs every six hours to 1,440 sets of vital signs a day. It's given to the staff with AI running in the background, showing them trends that are developing.
How is your wearable technology different from others that monitor patients’ vitals?
Everything we make in patient monitoring and sell is medical grade. And that's our belief: that decision making around patients wearing our devices requires all the things that go along with being medical grade, which means robust design, commitment to regulator partners to meet and exceed their standards, and our own internal standards. So that when we put a device on someone at the bedside, we know it's going to perform at a very, very high level, with accurate data trending very, very rapidly. That's what we're used to at the bedside.
We also know that there's a consumer space that is growing very fast with non-medical grade devices, and we're not interested in that space. We firmly believe that as the medical complexity of decision making increases around patients that are wearing wearables, that a medical grade device will be foundational to the care of those patients. So everything that we've got is medical grade, and when we look at wearables for remote patient monitoring in and outside the hospital, we want our healthcare provider partners to know that they're getting the same quality and same performance that they're used to in all of our other patient monitoring devices.