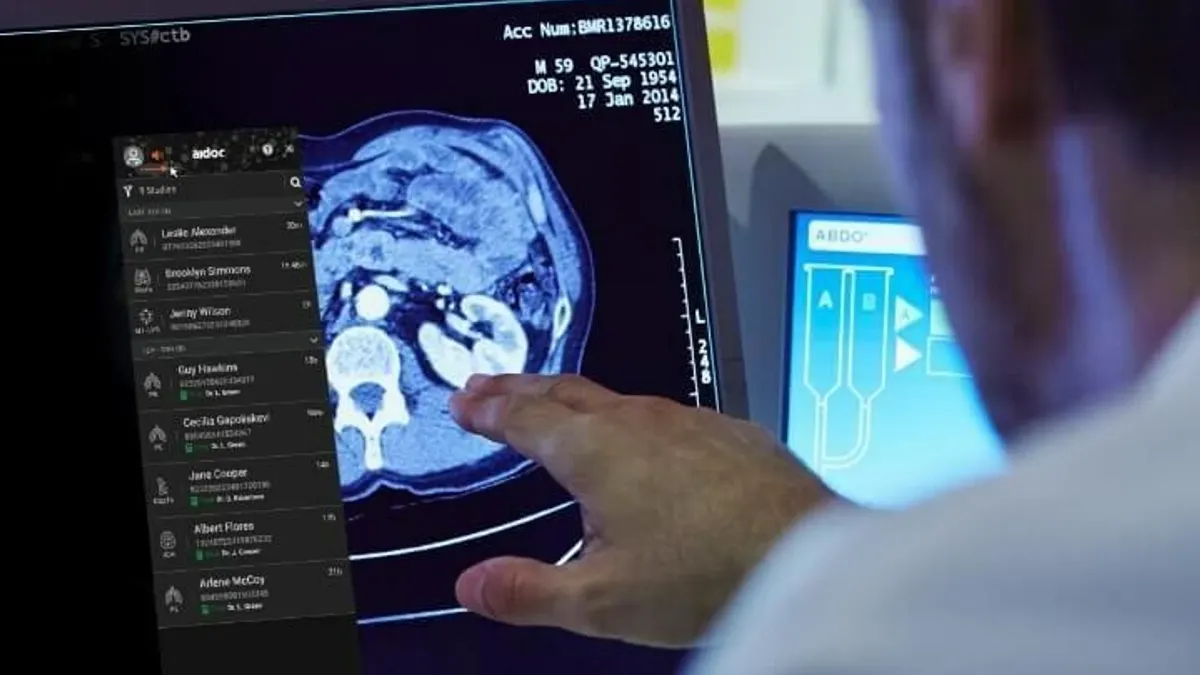
The Federal Communications Commission on Wednesday approved the final round of provider applications for funds to furnish telehealth in their communities, exhausting the $200 million program just as COVID-19 cases surge over the 3 million mark in the U.S.
Of the 539 nonprofit and public health providers that received taxpayer money from the program since its start in April, 21 providers received $1 million each from the program, including huge hospital systems that bring in millions, if not billions, in annual revenue.
Months into the pandemic, it's now a familiar criticism of how the Trump administration has allocated federal aid within the health sector. Behemoth for-profit operators and nonprofit systems with huge cash reserves have received the lion's share of $175 billion in bailout funds from the massive Coronavirus Aid, Relief, and Economic Security Act passed in March.
Though FCC didn't anticipate awarding more than $1 million to a single applicant in the COVID-19 Telehealth Program, "whether in one application, or across several applications," per the program's FAQs, West Coast powerhouse hospital system Providence received almost $2 million across four rounds of funding, a Healthcare Dive analysis of the recipients shows.
Providence, the country's third-largest nonprofit with 51 hospitals across seven states, was awarded $1 million in funding on June 3. One week later, it was awarded $866,750 for "connected COVID-19 kits to include tablets, Bluetooth thermometers, blood pressure monitors, and pulse oximeters, as well as connected stethoscopes," per an FCC release.
On June 17, Providence received another $105,000, and on July 1, Providence's flagship hospital, Providence Regional Medical Center in Everett, Washington, got $19,736 for a "laptop computer and videoconferencing equipment" to remotely treat COVID-19 patients quarantined at home with "already provided thermometers and pulse oximeters."
A Providence spokesperson told Healthcare Dive many of its patients live in rural areas, and the funds are necessary to treat and monitor infected patients in their homes, lowering the chance of virus transmission and conserving in-demand personal protective equipment in its hospitals.
"When applying for the FCC grants, we consolidated our applications as a single health system, and we validated with the FCC directly that these awards were not received in error," the spokesperson said. "We further confirmed they were aware that their grants had been awarded to various entities within our single health system."
"This was intentional and the awards to that Consortium cover dozens of hospitals across the country" an FCC spokesperson told Healthcare Dive.
But Wednesday's release raises questions about whether the brunt of the $200 million pot flowed to nonprofit and public health providers with greatest need, researchers say.
"While there are many smaller clinics and health systems that were supported by this program, my eyebrows were raised when I saw that many payments, in particular the largest payments, went to large academic health systems," Ateev Mehrotra, an associate professor of healthcare policy at Harvard Medical School, told Healthcare Dive.
"Many of these larger systems already had ample resources and well-developed telehealth programs. One worries that the money went to health systems with the capacity to write an application for the money rather than the providers who needed it most," Mehrotra said.
Providence, which reported income of $1.36 billion in 2019 and received $509 million in CARES grants, has extensive telehealth infrastructure that ran almost 70,000 patient visits last year and was able to scale up to 70,000 visits a week amid the pandemic. It's been building out that infrastructure for more than 12 years, focusing on highly acute inpatient scenarios like teleICU, telestroke and telepsychiatry.
Many of the 21 providers that received $1 million in taxpayer dollars are elite, tech-savvy systems with huge amounts of assets, better situated than other providers to ride out the pandemic, such as Minnesota-based academic medical center Mayo Clinic, which brought in income of more than $1 billion last year and received $220 million in CARES grants.
Other $1 million recipients included 11-facility public system NYC Health + Hospitals, Connecticut integrated system Yale New Haven, Baltimore-based Johns Hopkins Health System and four-state network Novant Health. Another large regional system, Pennsylvania-based Geisinger, received almost $979,000.
Mayo Clinic, Novant, Johns Hopkins and Geisinger facilities were named some of the "most wired" hospitals in the U.S. for their tech and IT capabilities last year by health IT group CHIME.
FCC says it selected applicants based on their goals for the funding, the conditions they were treating and whether the funding was targeted to high-risk populations or strained geographic areas facing provider shortages, hospital closures or limited broadband access.
Myriad barriers, including a lack of technology or reliable internet coverage, make it difficult for patients to access virtual care services — especially those living in low-income, minority and rural communities.
But there's little overlap in regions affected the most by this "digital divide," and regions with providers that received funds in the FCC's telehealth program, the analysis shows.
Montana, for example, has the slowest average internet speed of any state, but was one of three states that received zero allocations, though Providence does operate in that state. Roughly one-third of Montana citizens don't have reliable broadband coverage.
Likewise, only one in seven Utah households has an internet subscription, but the state's providers received just over $1 million in funding — the same as Mayo Clinic, magnifying concerns the telehealth rush spurred by the pandemic could exacerbate existing health and digital disparities.
How much each state received from the program
Z
A
FCC has taken strides to address the digital divide. Earlier this month, the agency added $198 million to a program meant to tackle those issues for rural healthcare providers, though some researchers think the FCC could do more to improve computer ownership and Internet access in rural and low-income communities.
Providers of all sizes and specialties have scrambled since March to round out their virtual care capabilities to recoup revenue and provide continuity of care for their patients, many of whom are leery of in-office visits due to the potential for virus transmission. Implementation can be labor intensive and pricey: thousands of dollars, depending on the vendor and size of the practice.
The COVID-19 Telehealth Program was created by the CARES Act to stimulate virtual care infrastructure and access. The program, which passed the $100 million mark mid-June and stopped accepting new applications on June 25, issued 14 total rounds of funding over its lifespan, with an average allocation size of almost $370,400.
The majority of allocations — 150 — didn't go above $100,000.
Leyden Family Service and Mental Health Center in Franklin Park, Illinois, received the smallest amount: just $1,468 to buy phones, wireless data plans and videoconferencing software to provide remote behavioral health treatments and try to keep patients out of the area hospital's emergency room.
Overall, providers that got funds span 47 states and Washington, D.C. Along with Montana, Alaska and Hawaii were the odd states out, with no providers allocated funds.
New York, the state hardest hit by COVID-19 so far, received the most money from the program by a landslide: $32.5 million across 74 providers, more than 16% of the overall pot and roughly triple the next-closest state, Ohio. However, New Hampshire providers received the largest allocations on average.
Providers in New York and California, the states with the majority of confirmed COVID-19 cases, benefited most from the program
FCC Chairman Ajit Pai called the program a "success" in a Wednesday statement. But much like other Trump administration stimulus funding programs, it's been dogged with accusations of mismanagement.
Despite a sum $33 million in approvals by late May, only one provider had actually received their allocated funds, sparking requests from Democratic lawmakers for more transparency.
FCC leadership chalked the delay up to the approval process. To receive disbursements in the program, providers must submit an invoice and supporting documentation for the costs of eligible devices and services, as a check against waste and abuse. However, the process may have had the unintended effect of adding administrative burden on already stressed providers, slowing down the process when practices and hospitals need federal aid in hand as soon as possible.
"Participants have been making those filings in recent weeks and Commission staff is reviewing those filings and approving them as appropriate," an FCC spokesperson told Healthcare Dive.
The agency did not answer questions about how many providers had received their allocated funds, or how much money had gone out the door so far.