Dive Brief:
-
FDA on Wednesday announced availability of a tool newly endorsed by the agency to help developers of automated insulin dosing systems consider a technology's impact on quality of life and psychosocial functioning in people with Type 1 diabetes.
-
The tool is a set of questionnaires meant to gather patient and caregiver perspectives on using automated insulin dosing systems, which combine a continuous glucose monitor (CGM), an insulin pump, and an algorithm that takes glucose values from the CGM and insulin pump dosing history to automatically direct the pump's dosing. It's the latest qualification in FDA's voluntary Medical Device Development Tools (MDDT) program — a relative rarity, with the agency listing just six such designations since issuing guidance on the program in August 2017.
-
The move by FDA comes on the heels of the American Diabetes Association's annual Scientific Sessions, where quality of life improvements from automated insulin delivery systems, including one combining an interoperable Tandem algorithm and pump with a Dexcom CGM, were a key technology of interest.
Dive Insight:
The qualification of the development tool is FDA's latest show of support for customizable, automated insulin dosing systems. The agency has supported advancement of the systems in recent years, including multi-vendor interoperable versions, developing a path to market for the systems via a series of De Novo authorizations.
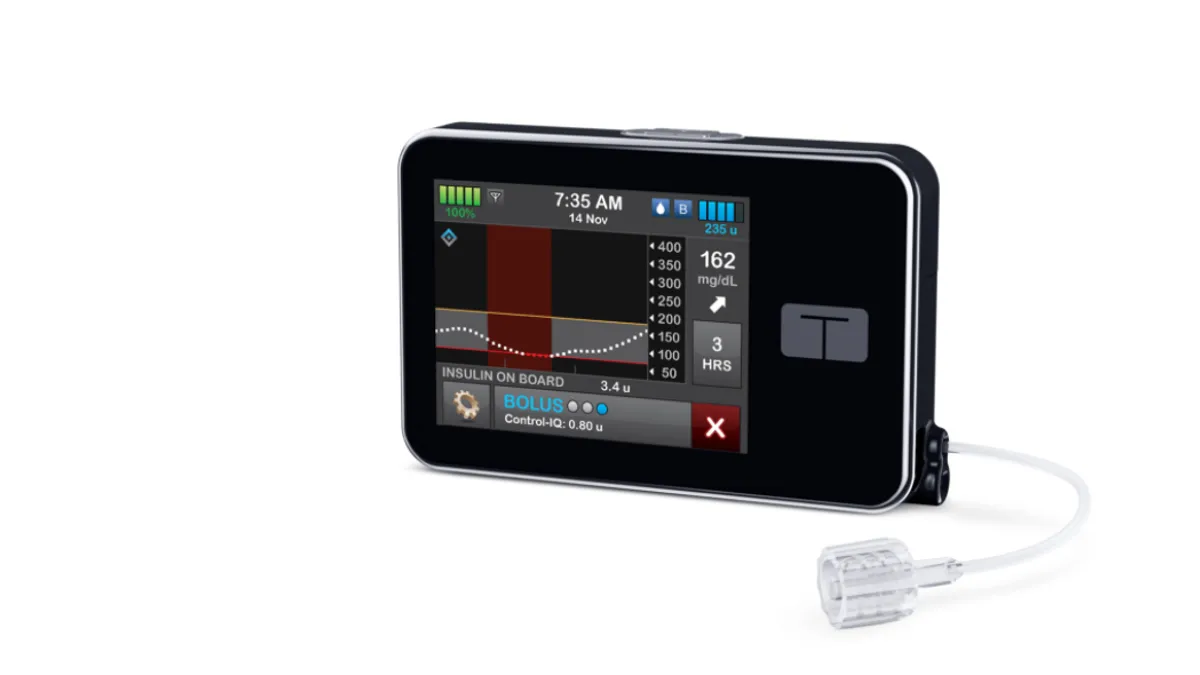
Tandem Diabetes' Control-IQ algorithm was the first automated glycemic controller authorized by FDA. It's meant for use with Tandem's interoperable pump, the first alternate controller enabled (ACE) pump OK'd by the agency, and Dexcom's G6 CGM, the first device deemed an integrated continuous glucose monitor (iCGM).
Tandem presented quality of life data for its Control-IQ earlier this month at ADA's virtual Scientific Sessions. And as the safety and efficacy of automated insulin dosing systems grow more established, additional research will likely be focused on patient-reported outcomes and overall quality of life, as well as more specific metrics like quality of sleep, said Tandem behavioral scientist Steph Habif in an ADA interview with MedTech Dive.
The baseline and post-intervention questionnaires are meant for use with either youth or adults with Type 1 diabetes, as well as partners, parents or caregivers. They assess factors like the system's effects on glycemic control, daily activities, social activities, and short and long-term complications, as well as device reliability and ease of use. Development of the tool was spearheaded by U.K.-based researcher and psychologist Katharine Barnard-Kelly.
The MDDT program aims to identify scientifically validated methods, materials or measurements that can assess safety, effectiveness or performance of a medical device to help with device evaluation and support regulatory decision-making, according to the FDA's guidance.
Other tools qualified over the last year or so include a statistical data tool meant to help developers of active implantable medical devices prepare safety test results; a material to help assess the effects of high intensity therapeutic ultrasound devices before testing them in humans; and a biomarker test to help develop treatments for traumatic brain injuries.