Dive Brief:
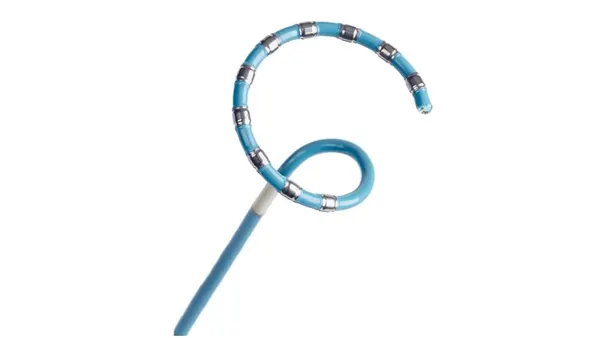
- Abbott’s drug-eluting resorbable scaffold has improved outcomes in people with below-the-knee (BTK) artery disease, according to study data shared Wednesday. The New England Journal of Medicine published the results.
- After one year, 26% of people who received Abbott’s Esprit BTK had suffered negative outcomes such as amputation, compared to 66% of those who underwent angioplasty, causing the trial to meet its primary endpoint. Esprit BTK performed similarly to angioplasty on its safety endpoint.
- Based on the data, Abbott plans to submit Esprit BTK to the Food and Drug Administration for review, it said in a statement about the results. Authorization would give physicians an approved alternative to off-label interventions such as metal stents.
Dive Insight:
Existing options for the treatment of people with arterial disease below the knee have limitations. Earlier this year, a phase 3 study found angioplasty is superior to surgery, but the durability of the procedure is a problem. Mechanical scaffolding can overcome the limitations of angioplasty but creates its own issues, notably because it prevents remodeling of the vessel and is associated with late complications.
In theory, drug-eluting resorbable scaffolds could overcome these challenges. Like metal stents, resorbable scaffolds support the vessel and release a drug to stop the artery from narrowing again. The difference is that the scaffold is resorbed by the body over time, facilitating vessel remodeling and avoiding late complications.
Abbott failed to establish the resorbable technology in coronary artery disease, pulling its device from the U.S. market in response to low sales and safety signals one year after winning approval. But it initiated a trial in BTK patients in 2020. The company shared data from the Esprit BTK trial at the Transcatheter Cardiovascular Therapeutics (TCT) 2023 conference and in the NEJM.
The primary endpoint looked at freedom from amputation above the ankle of the target limb, occlusion of the target vessel, clinically driven revascularization of the target lesion and binary restenosis of the target lesion after one year. In the Esprit BTK cohort, 74% of patients were free from those outcomes, compared to 44% of their counterparts who underwent angioplasty.
That 30-percentage-point difference was big enough for the trial to find Esprit BTK is statistically superior to angioplasty. Esprit BTK was non-inferior on the primary safety endpoint, which looked at perioperative death and major adverse limb events at six months.
Abbott changed the primary efficacy endpoint after an interim analysis. The authors of the NEJM paper list the change, which added freedom from binary restenosis to the endpoint, as a limitation of the trial, but cite reasons for confidence in the data. Esprit BTK beat angioplasty on the original primary endpoint, which Abbott kept as a powered secondary endpoint, although the result was closer than on the revised endpoint.